Warning Signs Hidden in Your Atrial Fibrillation ECG That Could Save Your Life
Table of Contents
Every time your heart beats, it sends out a tiny electrical signal. That signal travels through the heart muscle in a precise sequence, triggering contractions that push blood forward through your body. When everything is working as it should, this sequence is clean, rhythmic, and predictable. But when the electrical system breaks down, as it does in atrial fibrillation, that breakdown leaves behind evidence. And that evidence is exactly what shows up on an atrial fibrillation ECG.
Atrial fibrillation, or AFib, is not a rare condition hiding in cardiology textbooks. It is the single most common sustained cardiac arrhythmia in clinical practice today, and its prevalence continues to climb alongside rising rates of hypertension, diabetes, and obesity across India and globally. Despite how common it is, a large number of people living with AFib have no idea they have it. The heart is misfiring, clots may be forming, stroke risk is building, and yet the person feels nothing unusual enough to act on.
This is precisely why understanding the atrial fibrillation ECG matters so much. It is the tool that makes the invisible visible.
At Sunfox, we build technology that puts cardiac monitoring into everyday hands. Part of that mission is making sure people understand what their heart data actually means. So let us walk through everything worth knowing about the atrial fibrillation ECG, from how to read it to why catching it early can fundamentally change outcomes.
The ECG: Your Heart's Electrical Diary
Before diving into what goes wrong in AFib, it helps to understand what the ECG is actually recording. An electrocardiogram captures the electrical activity of the heart by detecting tiny voltage changes through electrodes placed on the skin. These voltage changes are plotted over time, producing a waveform that reveals how the heart is functioning beat by beat.
Each cycle on a healthy ECG contains identifiable components. A small rounded wave appears first, followed by a sharp tall complex, and then a second gentler wave. These are referred to as the P wave, QRS complex, and T wave. Each one corresponds to a specific electrical event inside the heart.
The P wave is generated when the upper chambers, the atria, receive a signal from the heart’s natural pacemaker, the sinoatrial node, and contract in response. The QRS complex reflects the electrical activation of the lower chambers, the ventricles, which are responsible for pushing blood out into circulation. The T wave marks the electrical recovery phase before the next cycle begins.
In a normal atrial fibrillation ECG comparison, the healthy tracing shows these components appearing in a steady, regular sequence. The spacing between beats is consistent. Everything arrives on schedule. The atrial fibrillation ECG, by contrast, tells a completely different story.
Inside the Chaos: What AFib Does to the Heart
To make sense of the atrial fibrillation ECG, you first need to understand what is actually happening inside the heart when AFib occurs.
In a healthy heart, the sinoatrial node fires once per beat, sending a single organized electrical wave across the atria. That wave triggers a smooth, unified contraction. In atrial fibrillation, the sinoatrial node loses its authority. Instead of one organized impulse, the atria are bombarded by hundreds of disorganized electrical impulses firing simultaneously from multiple locations. The result is not a coordinated contraction but a rapid, chaotic quivering, a trembling rather than a squeeze.
This electrical anarchy in the atria has consequences throughout the heart. The atrioventricular node, which acts as a gatekeeper between the upper and lower chambers, is bombarded with far more signals than it can process. It lets some through and blocks others, but in no predictable order. The ventricles therefore contract in a completely irregular pattern, sometimes fast, sometimes slow, never consistent.
All of this internal chaos is faithfully recorded on the atrial fibrillation ECG. What was once an orderly electrical diary becomes a document of electrical disorder.
Reading the Atrial Fibrillation ECG: Three Things That Stand Out
When a cardiologist examines an atrial fibrillation ECG, they are looking for a combination of findings that together confirm the diagnosis. These three features define the atrial fibrillation ECG pattern and distinguish it from every other type of arrhythmia.
A baseline that will not stay still
On a normal ECG, the flat section between beats, the part before each P wave and QRS complex, is just that: flat and quiet. On an atrial fibrillation ECG, this section is not flat at all. It shows rapid, fine, irregular undulations called fibrillatory waves, or f-waves. These tiny, disorganized deflections represent the hundreds of chaotic electrical impulses firing through the atria simultaneously. They do not have a consistent shape or timing. They simply roll across the baseline in a perpetually restless pattern.
This is one of the first things that alerts a trained reader when looking at an atrial fibrillation ECG. Where there should be clean P waves, there is instead an irregular trembling of the baseline. The organized electrical signature of atrial contraction has been replaced by noise.
Rhythm that follows no rule
In every other type of normal or abnormal heart rhythm, there is some degree of predictability in when the next beat will arrive. Even in certain arrhythmias, you can identify a pattern. The atrial fibrillation ECG offers no such pattern. The QRS complexes appear at completely random intervals. One beat may arrive quickly after the last, the next may take noticeably longer, and the beat after that falls somewhere entirely different.
Physicians describe this as an irregularly irregular rhythm, which means not just variable but genuinely unpredictable. No mathematical formula can tell you when the next beat will come on an atrial fibrillation ECG tracing. This randomness is a direct consequence of the AV node randomly transmitting whichever chaotic atrial impulse happens to reach it at any given moment.
This finding alone is enough to make atrial fibrillation a serious diagnostic consideration, but it is the combination of this irregularity with the abnormal baseline that makes the atrial fibrillation ECG essentially unmistakable.
Variable ventricular rate depending on treatment status
The number of QRS complexes appearing per minute on an atrial fibrillation ECG can vary widely. In someone who has just developed AFib or is not yet on treatment, the ventricular rate may be quite rapid, often between 100 and 160 beats per minute, because the AV node is being overwhelmed with signals from the fibrillating atria. In someone being managed with rate-controlling drugs, the atrial fibrillation ECG may show a much slower ventricular rate, sometimes within what we normally consider the normal range of 60 to 100 beats per minute.
A critical point here is that rate control does not mean AFib has resolved. The atrial fibrillation ECG will continue to show the absent P waves and the irregular rhythm even in a well-medicated patient. The underlying electrical disorder is still present. Treatment has simply managed one of its consequences.
The Different Forms of AFib and What They Mean for Detection
Not everyone’s atrial fibrillation ECG looks the same in terms of when it can be captured, because AFib itself comes in several forms that behave quite differently over time.
Some people experience paroxysmal AFib, meaning it starts without warning, lasts for a period ranging from a few minutes to several hours, and then stops on its own. This form of AFib creates a detection challenge because the atrial fibrillation ECG may look completely normal during the periods between episodes. A ten-second recording taken in a clinic on a day when the patient is not having an episode will show nothing abnormal. This is one of the most common reasons AFib goes undiagnosed for months or years.
Persistent AFib is present for more than a week and does not self-terminate. When a patient with persistent AFib has an ECG taken, the atrial fibrillation ECG findings will be present and consistent across recordings taken at different times. There is no window of normal rhythm to capture.
Long-standing persistent AFib refers to continuous AFib that has been present for over a year. At this stage, the heart has often adapted structurally to the ongoing rhythm disturbance, and the atrial fibrillation ECG may reveal additional findings related to those structural changes alongside the core AFib pattern.
Permanent AFib is a clinical decision point rather than a description of the ECG. Once a patient and their doctor agree that restoring normal rhythm is not the goal, the atrial fibrillation ECG will always show AFib findings, and the focus shifts entirely to rate management and stroke prevention.
Why Early Identification of the Atrial Fibrillation ECG Pattern Is Critical
Recognizing an atrial fibrillation ECG is not simply a matter of academic interest. It carries direct, measurable consequences for a patient’s health trajectory.
When the atria are quivering rather than contracting properly, blood does not move through them efficiently. In certain parts of the atria, particularly a small pouch called the left atrial appendage, blood can pool and stagnate. Stagnant blood clots. Those clots can then travel through the circulation and lodge in cerebral arteries, causing a stroke. AFib-related strokes are often more disabling than other types, which makes early identification of the atrial fibrillation ECG pattern all the more important for getting patients onto appropriate anticoagulation therapy before a stroke occurs.
Beyond stroke, untreated or poorly managed AFib can weaken the heart muscle over time, contribute to heart failure, and significantly diminish quality of life through persistent fatigue, breathlessness, and reduced capacity for physical activity. None of these outcomes are inevitable. They are largely preventable when the atrial fibrillation ECG is identified and acted upon promptly.
How Home ECG Technology Is Closing the Detection Gap
The traditional model of cardiac monitoring created a significant gap in AFib detection. Patients would visit a clinic, have a brief ECG taken, and if they happened to be in normal rhythm that day, the atrial fibrillation ECG would not appear. The episode might be dismissed as palpitations, anxiety, or fatigue. Months could pass before another recording captured what was actually happening.
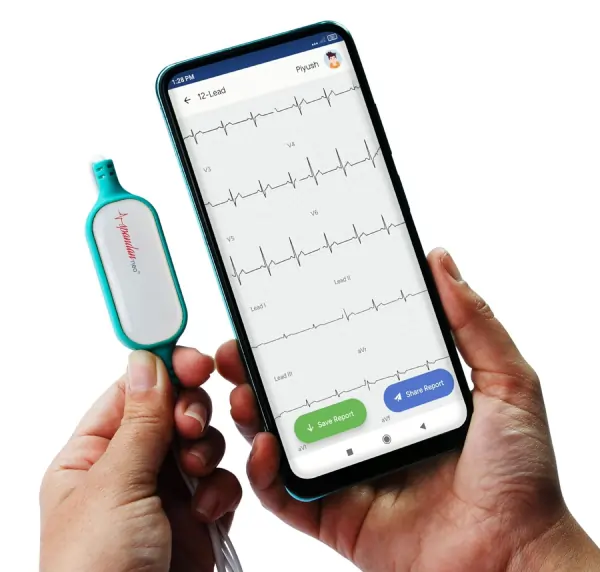
Modern portable ECG technology has fundamentally changed this equation. Devices like Spandan from Sunfox allow individuals to record a clinical-grade ECG in real time, from anywhere, at the exact moment symptoms appear. When someone feels an unusual flutter, an unexpected racing of the heart, or a sense of irregular beating, they can capture an atrial fibrillation ECG tracing immediately and share it with their cardiologist within seconds.
The diagnostic features that define the atrial fibrillation ECG on a hospital machine are equally visible on a Spandan tracing. The fibrillatory baseline, the irregularly irregular QRS pattern, the absent P waves, all of it appears with the same clinical clarity that allows a physician to make a confident interpretation. For people with paroxysmal AFib in particular, this kind of on-demand monitoring is the difference between capturing a diagnosis and missing it entirely.
Risk Factors That Make Regular Atrial Fibrillation ECG Monitoring Worthwhile
Not everyone has the same likelihood of developing AFib. Certain conditions and lifestyle factors substantially raise the risk, and people in these categories stand to benefit most from regular monitoring that can detect an atrial fibrillation ECG pattern before symptoms escalate into a cardiac emergency.
High blood pressure is the most common underlying condition associated with AFib development. The sustained pressure on the heart wall thickens and stiffens the atrial tissue over time, making it more electrically unstable. Diabetes affects blood vessel health and creates conditions that promote atrial remodeling. Thyroid disorders, particularly an overactive thyroid, can directly trigger AFib by accelerating the heart’s electrical activity. Obstructive sleep apnea exposes the heart to repeated episodes of low oxygen and pressure changes throughout the night, both of which destabilize atrial electrical behavior.
Chronic alcohol use, long-term obesity, a history of heart attack or heart failure, and structural heart disease all compound AFib risk. In individuals with one or more of these conditions who are not yet diagnosed with AFib, periodic atrial fibrillation ECG monitoring offers a practical and non-invasive way to screen for a condition that may otherwise announce itself through a stroke.
What Happens After an Atrial Fibrillation ECG Confirms the Diagnosis
A confirmed atrial fibrillation ECG is the starting point for a structured clinical evaluation and treatment plan. Your doctor will typically assess your stroke risk using a standardized scoring tool that accounts for factors like age, blood pressure, diabetes, and prior stroke history. Depending on that score, anticoagulation medication may be recommended to prevent clot formation.
Beyond stroke prevention, the next question is whether to attempt rhythm control, meaning restoring normal sinus rhythm, or rate control, meaning simply keeping the ventricular rate manageable while allowing the AFib to continue. Rhythm control strategies include electrical cardioversion and catheter ablation. Rate control relies primarily on medications.
The right approach depends on multiple factors unique to each patient, including how long AFib has been present, what symptoms it is causing, whether there is underlying structural heart disease, and the patient’s overall health and preferences. Ongoing monitoring with periodic atrial fibrillation ECG recordings remains essential throughout treatment to track whether rhythm control is being maintained or whether rate control is adequate.
Closing Thoughts
The atrial fibrillation ECG is one of cardiology’s most consequential diagnostic tools. It transforms an invisible electrical disorder into a visible, interpretable pattern that can guide treatment, prevent stroke, and in the most direct sense, extend lives.
Understanding what the atrial fibrillation ECG shows, the chaotic f-wave baseline, the absence of organized P waves, and the unpredictable spacing of ventricular beats, puts patients in a better position to understand their own condition and advocate for the monitoring and care they need.
At Sunfox, we believe that access to your own cardiac data should not require a hospital visit. The atrial fibrillation ECG that could change your health outcome might be just one recording away. Give your heart the chance to tell its story, and make sure someone is listening.